Separating historical truth from myth is as hard in science as anywhere else. This article has several examples, including whether Darwin got his ideas from someone else, and a dispute about whether Semmelweis was really ignored after his discovery of the link between hand-washing and disease.

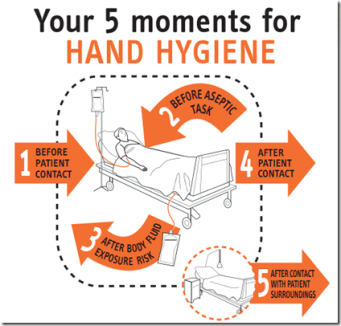
Semmelweiss teaches doctors to wash their hands c 1850 – it is still an issue today
The Hamblin article [about a supposed misplaced decimal point], unscholarly and unsourced, would become the ultimate authority for all the citations that followed. (Hamblin graciously acknowledged his mistake after Sutton published his research, as did Arbesman.)
In 2014, a Norwegian anthropologist named Ole Bjorn Rekdal published an examination of how the decimal-point myth had propagated through the academic literature. He found that bad citations were the vector. Instead of looking for its source, those who told the story merely plagiarized a solid-sounding reference: “(Hamblin, BMJ, 1981).” Or they cited someone in between — someone who, in turn, had cited Hamblin. This loose behavior, Rekdal wrote, made the transposed decimal point into something like an “academic urban legend,” its nested sourcing more or less equivalent to the familiar “friend of a friend” of schoolyard mythology. Source: Who Will Debunk The Debunkers? | FiveThirtyEight
I found a similar myth about aviation checklists. It’s a myth that they were invented because of the crash of a B-17 bomber prototype in 1935. The first B-17 checklist was in 1937, and by then many Navy aircraft had more complete checklists. Including one published before the 1935 crash.
As far as I could tell when I researched this, the B-17 checklist story was first told in a 1965 book by Edward Jablonski. Since then the myth has been passed from article to article to book, such as Atul Gawande’s generally excellent book, Checklist. The crash did happen, but checklists were invented independently of it.